This section presents the findings derived from the comprehensive analysis of the included studies, structured based on the data examined for each research question listed in “Research questions”.
Search results
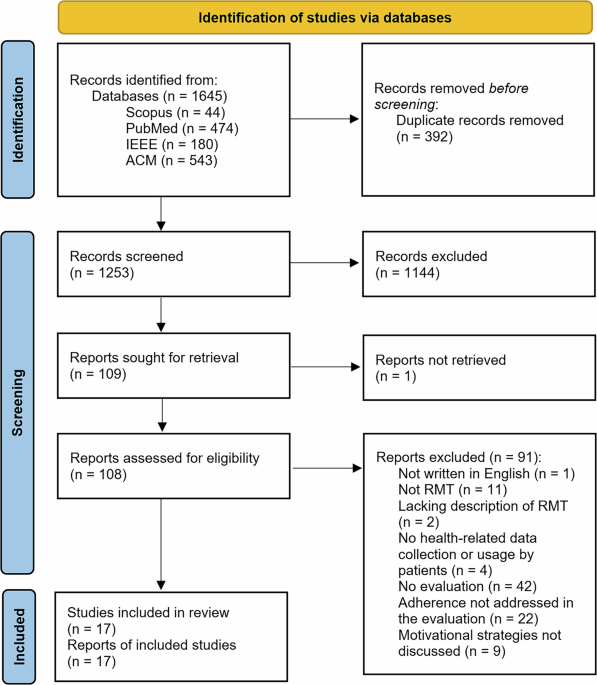
The initial search across four electronic databases returned a total of 1645 articles, of which 324 were identified as duplicates. The titles and abstracts of the remaining 1321 articles were screened, resulting in the exclusion of 1114 articles. As a result, 109 papers proceeded to full-text review. However, one paper could not be obtained in full text and was therefore excluded from the review. Based on the eligibility criteria, 17 studies were selected for detailed review and data extraction. The full screening process and the reasons for exclusion are summarized in Fig. 1.
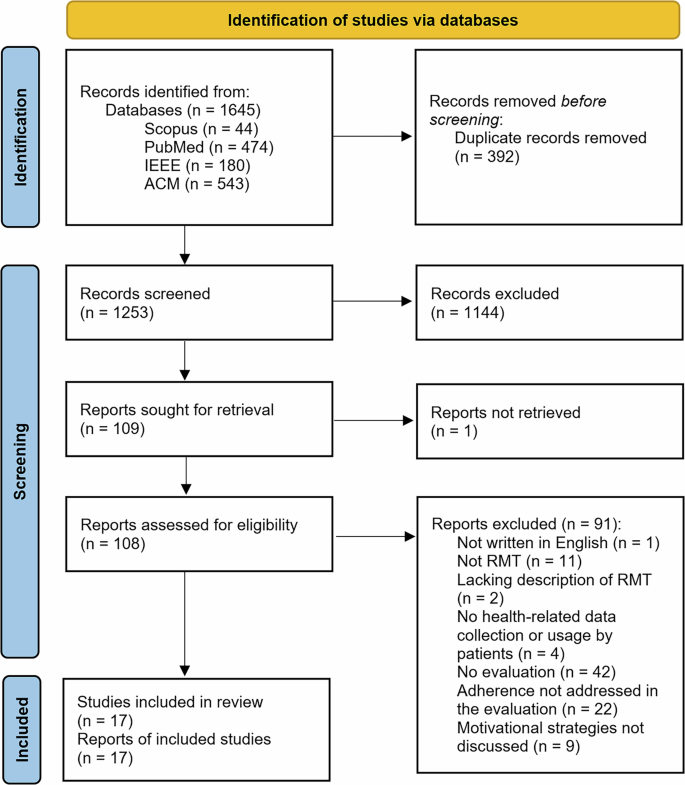
The PRISMA flow diagram illustrates the study selection process for this systematic review. Records retrieved through searches were assessed for relevance, with exclusions and reasons documented. Studies meeting the criteria were included in the final analysis.
Study characteristics
The 17 studies included in this review were published between 2011 and 2023, focusing on patients with diabetes and/or various CVDs. Geographically, 11 studies were conducted in the United States, with the remaining studies conducted in China (n = 1), South Korea (n = 1), Japan (n = 1), and Spain (n = 1). Additionally, one study was conducted across three locations: Spain, Italy, and the Czech Republic. These studies analyzed various types of RMTs and their associated digital interventions, employing diverse study designs, including six randomized controlled trials (RCTs), four pre-post studies, two longitudinal studies, two feasibility studies, one crossover study, and one formative in-situ evaluation study, with duration ranging from two weeks to 12 months. Sample sizes varied considerably, ranging from 1038 to 45039. 11 of the 17 studies (~65%) involved fewer than 50 participants, reflecting smaller-scale trials. The participant populations across these studies predominantly consisted of older adults. Detailed characteristics of each included study can be found in Table 1.
Digital interventions
Thirteen interventions in the included studies had multiple aims, primarily focusing on improving adherence to self-monitoring and management, such as medication intake and the tracking of symptoms and vital signs, like blood pressure and blood glucose levels39,40,41,42,43,44,45,46,47,48, to notice and focus on specific health problems. Six studies also emphasized adherence to lifestyle, including weight management, physical activity, dietary changes, and smoking cessation38,44,45,46,48,49. Two studies focused on the rehabilitation for motor deficits and the promotion of physical activity50,51. Additionally, many studies sought to empower patients by improving their self-efficacy33,41,45,47,52,53,54 and health literacy, as seen in42,45,47,53, educating patients about the fundamental disease knowledge, the risks associated with unhealthy behaviors, and the benefits of adopting healthy behaviors.
Interventions in the included studies take different forms and involve healthcare professionals on different levels. User control refers to interventions where patients have a primary role in managing their own care through digital interventions, including making decisions based on the data they collect and use. Expert control emphasizes the primary role of the healthcare professional, where they supervise the intervention and provide guidance to patients about their behavior. Among the interventions reviewed, 11 were based on user control38,39,40,41,42,43,46,47,50,51,53. These interventions allowed patients to manage their health independently, with minimal direct involvement from healthcare providers.
Five interventions incorporated both user and expert control33,44,45,49,52, where patients engaged in self-care activities while healthcare professionals monitored the tracked data and sent motivational or reminder messages at specific times. For example44, provided patients with control over daily medication management and adherence tracking, while healthcare professionals set up the medication plan and maintained communication with patients that facilitated ongoing support. Similarly, in45, patients were responsible for daily monitoring, goal setting, and accessing educational content, but healthcare professionals played a crucial role in guiding treatment, monitoring patient data, and adjusting care plans as needed. Additionally, one study48 employed two intervention groups: one with only user control, where patients input their self-care data (e.g., blood glucose, dietary habits, and step count), and another with both user and expert control, featuring bidirectional feedback from physicians.
The health-related metrics monitored in the RMT-based interventions include blood glucose levels, blood pressure, weight, symptoms, diet, physical activity, and medication adherence. 75% of interventions (n = 12) extended beyond mere data tracking by incorporating feedback mechanisms, ranging from real-time feedback to personalized and behavioral trigger messages. Additionally, nine interventions provided tailored educational resources, and one offered health reports to enhance user knowledge and support health management. Goal-setting and tracking features were included in six interventions. Moreover, reminders and alerts were integrated into six interventions each to support adherence and engagement. Social support, involving peer or family participation, was featured in two studies. Some of these also served as motivational strategies, which are further elaborated in Section “Motivational strategies to improve patient adherence”
This review identified 14 interventions that are based on mobile applications. Of these, four were smartphone-based38,40,41,51, one was implemented via a tablet33, and the remainder did not specify the type of device42,43,46,47,48,49,50,52,53. Additionally, two interventions were web-based39,45, while one was accessible through both web and smartphone interfaces44.
RMTs varied in their application across the studies. Four studies employed passive RMTs, such as pedometers, built-in accelerometers, and gyroscope sensors, to unobtrusively monitor physical activity without requiring user input from participants41,43,50,51. The majority of the studies (n = 9) utilized active RMTs, which necessitated higher levels of user interaction. These included mobile systems for time-stamped electronic logs, patient-reported physical activity outcomes, dietary records, and wireless monitoring devices, such as blood pressure monitors and weight scales33,38,42,44,45,46,47,52,53. Furthermore, four studies incorporated both active and passive RMTs, combining automated data collection with participant-reported metrics39,40,48,49.
Data plays a crucial role in the design and functionality of the digital interventions reviewed in this study. Across various interventions, the collected data from patients was used not only to record and monitor patient progress but also to personalize feedback, tailor messages, and assist care providers in decision-making. Eight studies specifically reported the use of graphical displays within the RMTs; details can be found in Table 2. Of these, three studies employed line graphs47,51,53, two used color-coded indicators47,48, and one utilized a horizontal bar display38 and two studies mentioned the inclusion of data visualizations33,45. These visualizations were intended to help patients track their progress over time and aid understanding of their health data. However, the limited descriptions of these graphical elements across the studies restrict our ability to fully assess their design and effectiveness in driving patient engagement.
Beyond data presentation, the collected real-time health data are used to generate personalized feedback40,47,50,51. For example, in ref. 47, collected weight data was used to trigger customized feedback, such as alert messages if the weight exceeded the standard. In ref. 50, the Yousician mobile application uses the device’s microphone to capture and assess the user’s musical performance, which triggers real-time auditory feedback from a keyboard with concurrent visual feedback on timing accuracy. Similarly, in ref. 51, both auditory and visual feedback are generated based on the collected data.
In six interventions, data are not only presented to patients but also shared with healthcare professionals to enhance monitoring, provide timely feedback, and support personalized care. For instance, the RehabPhone51 application employs cloud services to synchronize data across multiple devices, ensuring that both patients and healthcare providers can access and review long-term performance metrics. In ref. 33, the tablet application is complemented by a web portal where staff, such as community nurses and care managers, can monitor participants’ progress toward their goals. Through this portal, they can push text messages to patients’ tablets, offering informational or motivational content. Similarly, in ref. 44, patients can self-track their medication adherence, with data automatically sent to a website for professional analysis and communication with patients. In ref. 46, patient input data is uploaded to a system database, allowing doctors to remotely view the latest health records of patients. Two interventions45,48 link collected data with electronic health information systems. In ref. 45, an interactive web-based system was integrated with electronic health records (EHRs), enabling real-time monitoring and immediate response from healthcare providers. Similarly48, developed a mobile application that enabled physicians to view patient data in real time between clinic visits, incorporating lifelog data from personal sensors and wearables into electronic medical records.
Another two interventions38,49 use advanced data processing to provide more sophisticated feedback mechanisms. For example, in ref. 38, a statistical framework was used to provide real-time, personalized blood glucose forecasts by integrating self-monitoring data with physiological models, enabling continuous updates and more accurate predictions to assist patients in daily management tasks. Similarly, in ref. 49, both static data from a baseline database and dynamic behavioral data from patients were fed into a message-matching module to select appropriate messages tailored to the patient’s needs. This system also included a behavioral analysis module, which extracted information from the dynamic database to assess patient adherence and behavior, refining the feedback strategy. However, in four studies39,42,52,53, the collected data was used solely for recording purposes or study analysis without triggering any further actions within the intervention. For example, in52, the focus was more on recording patient-generated data rather than using it to trigger feedback mechanisms or alerts; in ref. 39, although data from pedometers was processed, it was used solely for study analysis and was not integrated into the intervention itself.
Motivational strategies to improve patient adherence
To understand the factors contributing to increased adherence to patients’ self-care behavior, we analyzed the motivational strategies employed in each study. These strategies can be broadly categorized into seven types: feedback, reminders and motivational messages, goal setting and tracking, social interaction, health literacy, reward, and gamification. Multiple motivational strategies were often combined to enhance user engagement and adherence. Details on applying these strategies and the related theoretical underpinnings in each intervention are presented in Table 3.
Twelve interventions provided personalized feedback to patients on their behavior and performance related to self-care, often also including alerts or recommendations38,39,40,46,47,48,49,50,51. For instance, in ref. 38, personalized blood glucose forecasts were offered to assist with meal-time decisions, which patients found reassuring and motivating, with one participant mentioning, “It would also tell me when I was doing wonderful. I am taking care of my sugar.” In ref. 46, a health check-up module was included to analyze blood pressure trends and hypertension grades, providing tailored feedback. In ref. 51, the feedback module delivered auditory cues, such as compliments and fanfare sounds, and visual feedback based on performance metrics after activity completion. This approach is akin to that used in ref. 50, where the Yousician mobile application captured musical interactions and triggered real-time auditory feedback from a keyboard, coupled with visual feedback on timing accuracy. Additionally, in ref. 43, text messages were sent to reflect patients’ recent self-monitoring blood glucose frequency and glycemic control, with examples like, “You are doing a good job of monitoring. Your blood sugar levels are improving.” However, this study highlighted a potential downside: motivational messages could sometimes be discouraging, particularly when feedback indicated that the intended behavior change had not been achieved.
Nine studies40,42,45,46,47,48,49,52,53 addressed patients’ health literacy in self-care interventions. Four studies45,47,48,49 utilized one-way messaging for providing education and information. Two of these studies49, and 45, combined the feedback with educational content in the messages: one49 provided prescription recommendations and health tips, while the other45 offered web-based educational content and feedback through messaging. The other two studies47, and 48, sent messages covering topics, such as diet, sleep, stress management, and medication adherence.
Additionally, four studies42,46,52,53 integrated educational materials within intervention applications to improve patients’ health knowledge, awareness, and self-care behaviors. For example52, featured modules on diet, exercise, and self-management, delivered through videos and text files. 40 included a “CHF-info” module with 10 educational units focused on heart failure and related conditions.
Eleven studies provided reminders and/or motivational messages to increase patient adherence33,39,40,41,42,44,46,47,48,52,53, included automated reminders40,41,44,53, patient-set reminders33,39,46, and personalized reminders arranged by external parties39. For instance, in ref. 46, a reminder service module was implemented, where the reminder times were initially set according to the management plan, with results indicating that this feature was particularly beneficial for patients with limited self-management experience, helping them complete daily tasks. Similarly, in ref. 40, the application sent real-time custom automated reminders to patients, prompting them to check their weight and complete HF symptom assessments. Although the intervention did not significantly enhance medication adherence, it notably increased self-care confidence compared to a control group that only received HF education.
Motivational messages were utilized in seven of these studies39,41,42,44,47,48,52. These messages, also referred to as reinforcement or behavior-triggered messages in some studies, were pervasive, being used to encourage adherence in various contexts39,41,42,44,47,48. For instance48, automatically sent motivational text messages alongside educational and behavioral content, while ref. 41 provided tailored motivational and reinforcement messages based on patients’ previous day’s medication adherence. In ref. 39, patients were invited to write personal motivational messages to be sent weekly or monthly, reinforcing their commitment to becoming more active. Additionally, in ref. 52, two types of motivational messages were used to send to participants based on the Fogg behavior model (FBM)55: “sparks,” which motivate those needing encouragement, and “facilitators,” for individuals lacking ability or capacity. The study found that spark triggers prompted specific behaviors more quickly than facilitator triggers or no triggers, although the difference was not statistically significant. However, the quicker response to spark triggers highlights their potential as a crucial element in prompting timely behavior, aligning with FBM’s emphasis on the need for motivation, ability, and a trigger to complete a task52,55.
Goal setting, as a commonly used motivational strategy, has been observed in six included studies33,39,45,48,52,53. Goal setting is often combined with planning and visual indicators for progress tracking33,53. In ref. 48, researchers set goals for patients to encourage physical activity. In contrast, in refs. 33,39,52,53, the goals are set by the users themselves. Participants in ref. 39 reported that while aiming to meet or exceed step goals was motivating, the fear of failing to meet these goals also drove motivation. Similarly, significant improvements were observed in ref. 53 in self-efficacy through goal setting, which likely enhanced participants’ confidence. The intervention in ref. 33 was specifically designed to support goal-oriented care with three modules: goal elicitation, goal setting, and goal tracking, designed to address autonomy, competence, and relatedness according to self-determination theory. Results indicated that, in practice, goal-setting and expectation management were predominantly assisted by care managers, which emphasized that digital interventions are often more effective when supplemented with human support33,56.
Social interaction is featured in four studies, which involved interaction among peers33,46 or between patients and their supporters, such as friends, family members, or healthcare providers39,43. For example, the application developed in46 employed a leaderboard feature that allowed users to compare their progress with others, thereby utilizing social support as a motivational tool. Similarly, social support was incorporated in33 by allowing users to view goal lists set by others within their social network. Participants found this feature informative and helpful, suggesting that integrating social network insights into digital interventions can enhance user engagement and trust33. In ref. 43, it was demonstrated that pairing adults with Type 2 diabetes with a patient-selected supporter in a mobile information and communication technology (ICT) intervention not only enhanced emotional and instrumental support, improving patients’ self-efficacy but also provided supporters with valuable insights and awareness about the challenges faced by diabetes patients, helping them more effectively reinforce positive behaviors in their paired patients. Additionally, in ref. 39, the program did not directly facilitate social interaction but offered resources, such as online links to local support services and encouraged users to create and share personal ’physical activity challenges’ with their social network, aiming to foster and strengthen social support networks.
In ref. 46, a leaderboard module was implemented in the designed mobile health application, using persuasive technology57 by motivating users to aim for higher scores to see their names on the leaderboards. This not only provided a competitive edge but also served as a source of social support, boosting motivation and indirectly improving compliance. Moreover, the health report module described in46 implemented a scoring system based on task completion and changes in health data, with the results indicating that patients who were more educated and motivated to learn about their condition found this module particularly effective in enhancing their compliance with prescribed treatments.
The reward strategy was employed in two studies33,50. In ref. 33, participants earned virtual crowns and trophies for their efforts, which they found motivating. Interestingly, the study33 also implemented negative rewards by using sad face icons when goals were unmet. Some participants reported that these negative rewards were also motivational; to avoid seeing a negative icon on their dashboards, they worked harder to achieve their goals33. However, some desired more tangible incentives, such as vouchers. In ref. 33, participants unlocked new levels and earned “stars” and “certificates” as rewards, displayed on a summary screen. The music-based nature of the intervention50 also provided an enjoyable and rewarding experience, enhancing engagement in rehabilitation.
Theoretical foundations in motivational strategies
Not all studies specified the theoretical underpinnings for the aforementioned motivational strategies. 41% (n = 7) of them did not explicitly mention the application of psychological theories, models, or principles in the design or implementation of their interventions. However, many of these strategies inherently align with well-established theories employed by the other studies.
The remaining ten studies cited a total of eight different theoretical models and constructs. Self-determination theory (SDT)58 was referenced in three studies33,39,41, which posits that humans have three innate psychological needs: autonomy, competence, and relatedness. This theory primarily supported strategies related to goal setting and autonomous regulation, aiming to enhance self-efficacy and foster intrinsic motivation. Social cognitive theory (SCT)59 was cited in two studies45,52. In ref. 52, SCT was used to design and reinforce social modeling statements in educational videos to boost self-efficacy beliefs; one example was “others like yourself have been successful in managing their type II diabetes.” This was implemented alongside the FBM55 to develop trigger messages to coincide with the use of the RMT. The other study45 integrated SCT with the theory of planned behavior60 and the health belief model (HBM)61 to enhance the effectiveness of the intervention without clearly outlining the distinct contributions of each theory. Additionally, the HBM61 was used in ref. 53 to guide strategies to enhance self-efficacy through educational resources and to use goal setting and reminders for regular task performance. Situation-specific theory (SST)62 was applied in ref. 47, where it focused on self-monitoring of symptoms, health literacy, and self-efficacy. This theory guided the strategies of educational and motivational messages within the intervention. The IMB model27 was used in ref. 40 to combine information on HF self-management with the RMT as a healthcare coach to enhance intrinsic motivation and improve engagement. The model specifies that health promotion behaviors begin with health promotion information and motivation, which subsequently lead to the development of skills required to initiate and sustain these behaviors27.
Evaluation of patient adherence to self-care
Seventeen studies evaluated patient adherence to various self-care behaviors, including behavioral adherence to prescribed activities (n = 8), application usage/engagement (n = 6), and medication adherence (n = 3). Some studies40,42,47,48,49,53 assessed adherence to more than one activity. Sustained engagement over time is considered a dimension of adherence in this review, as it reflects consistent participation and serves as a facilitator of overall adherence63.
Adherence to application usage was normally assessed through the time spent on the applications40,46,50,52 and the frequency of usage across different features33,38. Medication adherence was evaluated in three studies, each employing distinct methods: one study40 used the self-administered Morisky medication adherence questionnaire, another44 utilized the proportion of days covered with medication along with the simplified medication adherence questionnaire (SMAQ), and a third study41 measured adherence based on the timing of medication intake relative to the prescribed dosing schedule. Nine studies focused on behavioral adherence to prescribed activities, including self-monitoring of vital signs (e.g., blood pressure, blood glucose levels, and body temperature)42,43,45,48,49,53 and dietary54, completion of educational content and quizzes53, and performing physical activity tasks39,48,51. Most of these studies measured adherence by assessing the frequency or degree to which patients followed medical prescriptions and their success in achieving set health goals. It was worth noticing that in ref. 49, they used a set of indexes to estimate the patient’s adherence to the treatments. Additionally, in ref. 47, the self-care of heart failure index (SCHFI) was used to subjectively assess adherence by evaluating participants’ self-care maintenance, management, and self-confidence.
In total, 59% of the included studies (n=10) reported high or increased adherence rates in their intervention with motivational strategies33,40,41,42,44,46,48,49,51,53. Among these, two RCTs showed significantly higher adherence in intervention groups compared to controls. The smartphone medication adherence stops hypertension (SMASH) intervention41 led to sustained medication adherence, highlighting the importance of self-efficacy and autonomous regulation. Similarly, in ref. 48, participants who received personalized feedback (MPC group) engaged more consistently with the app, although this engagement declined to 50% by the study’s end. Another three RCTs40,42,49 reported high adherence in the intervention groups, but results were not statistically significant or lacked p-values. In ref. 42, patients, including those with poor digital literacy, maintained high adherence to self-monitoring throughout the study, indicating the application’s sustainability. Two studies40,49 reported overall improvements in adherence, but they did not include detailed statistical information, such as p-values, to show whether these improvements were significant.
Two longitudinal studies reported user adherence exceeding 90%, indicating high levels of sustained engagement over time51,53. In ref. 51, patients preferred using their smartphones over traditional rehabilitation tools, though some technical issues affected adherence. In ref. 53, goal-setting and daily reminders in the application were found to significantly improve users’ self-efficacy and help establish effective hypertension management habits. A pre-post study44 showed increased adherence based on self-reports, though this was not reflected in medication coverage, suggesting the need for multiple adherence measurement methods. Additionally, over 60% of participants had a college or professional education, which correlated with higher adherence levels44. A formative evaluation33 revealed that participants who remained engaged valued rewards and experienced increased commitment to their health goals, while those who abandoned the application cited distrust, health issues, or technical difficulties as reasons for disengagement.
Other studies showed mixed results. A crossover study52 observed higher task adherence with behavioral trigger messages, though not statistically significant. Despite improvements in beliefs about physical activity in ref. 39, the results did not see increased activity levels at 12 months. Among the pre–post studies, usage remained stable over a three-week period in ref. 50, while45 provided engagement data without detailed results45; clinically relevant improvements in maintenance, self-management, and self-confidence were observed in ref. 47, though these results lacked statistical significance. In feasibility studies, one43 found that 20 to 30% of participants did not adhere to SMBG, and the other38 noted a decline in adherence overtime during the intervention.
link








