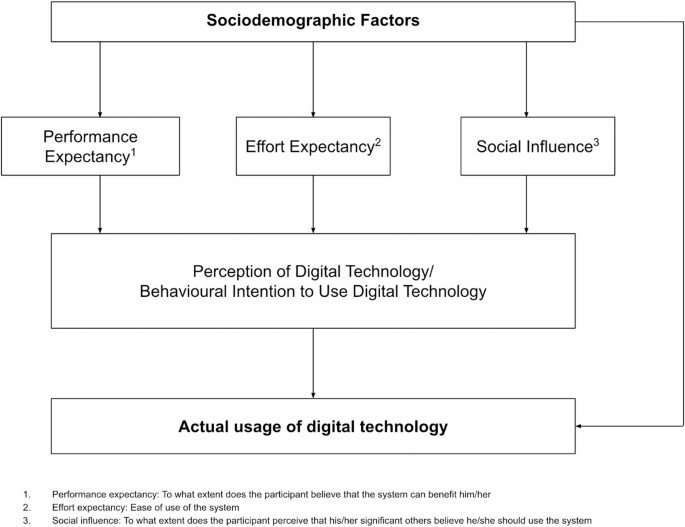
Our study showed that increasing age, being unmarried and occasional access to technology are key barriers to using digital technology in chronic disease management. Conversely, having higher education and higher income are key facilitators. Higher income, good PE and SI were consistently associated with digital technology usage.
Our study found older age was associated with a poorer perception of digital technology in chronic disease management. Likewise, a previous study showed older individuals had lower self-efficacy and higher anxiety rates regarding digital technology use26. Decline in cognitive abilities, steep learning curves and physical, functional, visual limitations also hamper their adoption of new technologies26,27. As such, they demonstrate lower digital literacy and proficiency, resulting in poorer perceptions of technology, translating to poor usage as per the UTAUT model17. A study in Singapore further corroborated that health-seeking behaviour among older adults was not technology-centric, but leaned towards seeking direct medical care11.
In our study, occasional access to technology was associated with poorer PE and SI. Studies have shown that low perceived usefulness leads to decreased usage of digital health technologies which begets social isolation, potentially causing lower awareness of digital health technology and missed health announcements28,29. Hence, occasional access to technology is a barrier for use of digital technology in chronic disease management. This is consistent with a previous study that shows habitually using technology increases technology usage for other purposes, including digital health30.
Our study found that being married was associated with higher EE and SI. A previous study found that married individuals experience greater social support from their partners compared to other relationships31. This explains our findings where married participants experienced higher SI than unmarried individuals. Moreover, their children may provide digital assistance to their parents, facilitating ease of use, thereby increasing their EE32,33.
In our study, higher education was associated with better PE and perception. Previous studies reported that higher education is linked to higher cognitive function, contributing to greater skills acquisition capabilities34,35. These individuals have greater propensity to appreciate digital health technologies in managing their chronic disease, translating to a higher PE and better perception, predisposing to greater usage.
Higher income was another key facilitator for higher PE and usage of digital technology in our study. This is consistent with previous studies which reported positive attitudes and greater receptiveness towards digital technologies in higher income groups; due to greater access and exposure36,37,38,39. This predisposes to greater PE, facilitating greater usage.
These findings have critical policy implications for improving digital health adoption among older adults, particularly in addressing barriers related to age, education, and income. Policymakers can implement targeted initiatives such as subsidising digital devices and providing affordable or free access to digital health platforms to alleviate financial constraints for lower-income individuals. Additionally, bridging the digital literacy gap through community-based, multilingual education programmes and workshops tailored to older adults can enhance confidence and familiarity with digital health tools27. Integrating blended care models, where digital health technologies complement traditional face-to-face interactions, may facilitate gradual adoption among those less familiar with technology40. Public health campaigns should emphasise the benefits, ease of use, and security of digital health technologies to build trust and increase acceptance, leveraging healthcare professionals and community organisations for effective outreach41. Emphasising the necessity of user-centred design, ensures that digital health platforms are intuitive, accessible, and seamlessly integrated with existing healthcare infrastructure. Special attention should be given to usability among older adults, including simplified interfaces, voice-assisted navigation, and multilingual support. Additionally, platforms must be designed to enhance interoperability with existing hospital systems, minimising disruptions in clinical workflows and maximising adoption among healthcare professionals42. By implementing these policy-driven strategies, digital health adoption can be scaled equitably, ensuring that older adults and underserved populations are not left behind43.
By incorporating these insights into policy, healthcare operations, and technology development, digital health adoption can be optimised, ultimately leading to better patient outcomes and improved healthcare efficiency. Future research should continue to build on this foundation by exploring longitudinal impacts and refining implementation strategies to provide evidence-based recommendations for sustained and inclusive digital health integration. Policymakers could promote subsidising of digital devices and community-based digital literacy programs in lower-income areas. In addition, targeted digital literacy and training programs for older adults or those with lower educational attainment may aid bridging the digital divide. Likewise, addressing concerns about data privacy and trust, as identified in our survey, may involve transparent communication about data protection practices and the development of trusted digital platforms. These measures could help enhance the usage profile of digital health technologies across diverse population groups.
Strengths and limitations
The main strength of our study was the usage of the UTAUT model and validated SEMCD scale to measure perception towards digital technology. Both models provided established and reliable measures of our outcomes and variables, increasing the objectivity, accuracy and potential translatability of our paper.
Although UTAUT provides a robust framework for understanding technology adoption, its application in the healthcare sector is subject to debate due to the multifaceted, interdisciplinary nature of healthcare systems. Unlike consumer-oriented technologies, healthcare innovations must accommodate organizational constraints, regulatory environments, and interprofessional collaboration, factors that UTAUT does not fully address.
While our study adapted UTAUT to offer valuable insights, future research should consider alternative or extended models that incorporate sociotechnical perspectives, recognizing the dynamic interactions between technical systems, healthcare professionals, and institutional factors. A previous systematic review has highlighted that patient adoption of digital health tools is influenced by a range of sociotechnical factors beyond those captured by UTAUT44. These include usability challenges, data privacy concerns, clinician-patient trust, integration with existing healthcare workflows, and the level of institutional support for technology implementation. Expanding the theoretical framework in future studies could provide a more holistic understanding of facilitators and barriers to adoption in healthcare contexts.
Another strength lay in our systematic and rigorous approach in conducting interviews. Interviewers meticulously documented the blocks visited and maintained a live, shared manual response tracking sheet of units which responded, denied response or did not answer, requiring repeat visiting. Thorough examination of all units within each block further eschewed duplicate responses. Moreover, the use of electronic devices to conduct surveys minimised interviewer bias.
Limitations of our study include: First, comorbidity status was assessed at an aggregate level, meaning that we did not differentiate between specific chronic conditions. While this approach allowed us to analyse general trends in digital health adoption, it may not capture condition-specific barriers and facilitators that could influence engagement with digital health technologies. For example, individuals with mobility-related conditions might face different adoption challenges compared to those managing chronic metabolic diseases. Second, the digital health needs and usability concerns may vary depending on the severity and progression of a condition, which was not accounted for in our assessment. Future studies should consider examining adoption patterns across specific chronic conditions to provide more targeted insights into disease-specific digital health interventions. Third, the use of voluntary sampling may introduce non-response bias, as responders might differ in sociodemographic characteristics from non-responders. The exclusion of residents from private housing, comprising 20% of the population (63), may also impact the overall sample representation of the population, threatening internal validity. Fourth, confinement to the Singapore population with a small sample size (n = 306) limits generalisability and external validity. Fifth, although the questionnaire was electronically self-administered in a face-to-face setting, administrators were available to provide minimal assistance when required, such as helping participants navigate technical issues. This design choice allowed us to simulate typical interactions with digital platforms. However, it may have introduced selection bias by favouring individuals with a baseline level of digital literacy. Future studies could consider alternative administration modes to ensure inclusion of participants with minimal or no digital experience. Sixth, while the UTAUT framework enabled us to systematically assess perception and engagement patterns, future research employing qualitative or sociotechnical approaches could better elucidate nuanced challenges—such as data literacy, personalization needs, and trust—in digitally mature healthcare environments. While this study identified key associations between sociodemographic characteristics and digital health perceptions, it does not capture the experiential or structural dimensions influencing use. Future qualitative studies are needed to deepen understanding of usability challenges, trust, personalization, and health system integration. Seventh, the use of the UTAUT framework and SEMCD scale inherently focuses on specific constructs of technology acceptance and self-efficacy, which do not fully capture the complex and multifaceted nature of digital health adoption in chronic disease management. This limitation suggests that the claims presented, while supported by the quantitative analysis, should be interpreted with caution. Future longitudinal and mixed-methods research are warranted to establish causal relationships and to explore broader contextual and experiential factors influencing digital health engagement. Eighth, modifications were made to the original UTAUT and SEMCD instruments, including the reduction of SEMCD from six to five items. As these changes were not accompanied by formal re-validation, our total scores cannot be benchmarked against normative data. This limits the generalisability and comparability of our findings. However, the retained items reflect the core dimensions of chronic disease self-management and remain relevant to the local digital health context. The score of 35 out of 50—equivalent to an average item score of 7—was interpreted as indicative of moderate to high self-efficacy within this population. Future studies should consider using formally validated adaptations to enhance the robustness and external validity of findings.
link








